Cervical Epidural Cortisone Injections
WHAT ARE CERVICAL EPIDURALS?
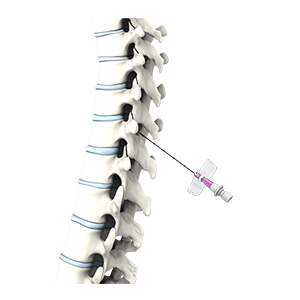
A cervical epidural is an injection of medication into the epidural space in the lower section of the cervical region to provide relief from pain or inflammation affecting the neck and upper back. The epidural space is the space between the outermost covering of the spinal cord (dura mater) and the wall of the spinal canal and runs along the length of your spinal cord. It is approximately 5 mm wide and is filled with spinal nerve roots, fat, and blood vessels.
HOW DO CERVICAL EPIDURALS WORK?
Cervical epidural cortisone injections are a mixture of anesthetic and steroid. Cortisone (a type of steroid) is a very powerful anti-inflammatory medication. By delivering an epidural injection directly into the cervical epidural space, the medication moves throughout this space, coating the inflamed or irritated nerve roots. The anesthetic functions by numbing the nerves to provide short-term or sometimes long-term pain relief and the corticosteroids act as anti-inflammatory agents providing long-term effects by decreasing the inflammation and irritation around the nerves.
INDICATIONS FOR CERVICAL EPIDURALS
Cervical epidurals are usually employed as a treatment when conservative measures, such as physical therapy or oral medications have failed to alleviate symptoms of pain or inflammation. Cervical epidurals are indicated to treat conditions, such as:
- Spinal stenosis
- Bulging or herniated disc
- Bone spurs
- Cervical radiculitis
- Failed cervical surgery (persistent pain despite surgery)
- Other injuries to the spine
PRE-PROCEDURE PREPARATION
Your doctor will review your medical history thoroughly before the procedure. You must inform your doctor about any health conditions you may have such as diabetes or bleeding disorders, and about any medications that you may be taking, such as blood thinners, over-the-counter medications, or supplements. You may be asked to stop taking certain medicines for several days before the procedure. You will be instructed not to consume any food or drink for several hours prior to the procedure.
PROCEDURE FOR CERVICAL EPIDURALS
A cervical epidural injection is performed as an outpatient procedure. You will lie down on the operating table on a face-down position. Your neck and upper back are sterilized with a cold antiseptic solution. The injection is performed using fluoroscopy (live x-ray images) to assist the doctor with the placement of the needle in the exact location to target the specific area causing the pain, so the patient can derive maximum benefit from the injection. X-ray dye is utilized to ensure that the spread of the injection is satisfactory. A small dressing is applied at the site of the injection to complete the procedure. Often, a light sedative is used, but heavy anesthesia is not recommended.
POSTOPERATIVE CARE
Post-procedure, you will be returned to the recovery area where you are required to stay for short time. You need to arrange for someone to accompany you post procedure as you will not be able to drive or travel back home yourself. If you have had sedation, you should not operate machinery, drive, or consume alcohol for 24 hours following injection. You need to adhere to instructions on pain medications and follow-up appointments to monitor your progress.
SIDE EFFECTS OF CERVICAL EPIDURALS
Some of the possible side effects of cervical epidural injections include:
- Pain at the injection site for a couple of days
- Fluid retention for a couple of days due to the effect of steroids
- Headache in some patients
- Risk of infection
- Facial flushing for a couple of days
- Menstrual periods may be affected in females due to the effect of steroids
Pre-Procedure Information
- These procedures are performed in an ambulatory surgery center under conscious sedation (anesthesia). Expect to avoid eating and drinking for several hours before the procedure – the ambulatory surgical center will inform you of specific guidelines.
- The following medications are “blood thinners” of one sort or another and must be avoided before the procedure:
Aspirin
Aspirin and all aspirin containing medications (Anacin, Ascriptin, Bayer, Bufferin, Ecotrin, Excedrin, Pentasa, and others) – Stop 7 days prior to your procedure.
All medications listed below should be stopped 3 days prior to your procedure:
NSAIDs (NON-STEROIDAL ANTI-INFLAMMATORIES)
- Choline and magnesium salicylates (CMT, Tricosal, Trilisate)
- Choline salicylate (Arthropan)
- Diclofenac potassium (Cataflam)
- Diclofenac sodium (Voltaren, Voltaren XR)
- Diclofenac sodium with misoprostol (Arthrotec)
- Diflunisal (Dolobid)
- Etodolac (Lodine, Lodine XL)
- Fenoprofen calcium (Nalfon)
- Flurbiprofen (Ansaid)
- Ibuprofen (Advil, Motrin, Motrin IB, Nuprin)
- Indomethacin (Indocin, Indocin SR)
- Ketoprofen (Actron, Orudis, Orudis KT, Oruvail)
- Magnesium salicylate (Arthritab, Bayer Select, Doan’s Pills, Magan, Mobidin,
- Mobogesic)
- Meclofenamate sodium (Meclomen)
- Mefenamic acid (Ponstel)
- Nabumetone (Relafen)
- Naproxen (Naprosyn, Naprelan)
- Naproxen sodium (Aleve, Anaprox)
- Oxaprozin (Daypro)
- Piroxicam (Feldene)
- Salsalate (Amigesic, Anaflex 750, Disalcid, Marthritic, Mono-Gesic, Salflex,
- Salsitab)
- Sodium salicylate (various generics)
- Sulindac (Clinoril)
- Tolmetin sodium (Tolectin)
This is a partial list. If you are unsure whether you are taking an NSAID, please call us.
Please notify our office if you are on any of the medications listed below. These will probably need to be held for several days prior to your injection.
- Warfarin (Coumadin)
- Acenocoumarol
- Heparin
- Low molecular weight heparin: Enoxaparin (Lovenox)
- Dalteparin
- Fondaparinux
- Clopidogrel
- Prasugrel
- Ticagrelor
- Cangrelor
- Dabigatran
- Rivaroxaban (Xarelto)
- Apixaban (Eliquis)
- Edoxaban
- Abciximab
- Eptifibatide
- Tirofiban
- You will need to be driven home from the procedure.
Post-Injection Instructions
- Rest at home for the remainder of the day following the injection. Don’t tackle any big projects. If you do experience aching in your neck or back, try an ice pack for 15-20 minutes or some of your usual pain medication such as Tylenol or Advil.
- The day after your injection you may resume normal activities but remember not to push beyond your limits.
- A follow-up appointment should have been scheduled before your procedure. If it was not scheduled, be sure to do so at the time of your procedure.
- Contact your doctor or the emergency room if you develop signs of infection (fever or redness at the site of injection), or if you notice a change in the way the nerves in your arms or legs are working (increasing numbness or weakness) or a change in your bowel or bladder function.
