Spinal Cord Stimulation
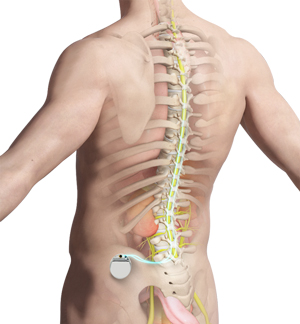
what is a spinal cord stimulator?
A spinal cord stimulator is a device that sends electrical impulses to the areas of the spinal cord causing pain and interferes with the transmission of pain signals to the brain. It blocks the brain's ability to sense pain in the stimulated areas, thus relieving pain without the side effects that medications can cause. The electrical impulses can be targeted to specific locations and, as pain changes or improves, stimulation can be adjusted as necessary.
indications for a spinal cord stimulator
Nerve compression or decompression can cause back and leg pain. Among other causes, scar tissue around the nerves or chronic inflammation of the nerves such as arachnoiditis may cause leg and back pain.
preparing for a spinal cord stimulator
Before implanting a permanent stimulator, you will undergo a trial stimulation period to see if the stimulation helps relieve the pain. If it does, a permanent stimulator may be implanted.
spinal cord stimulator procedure
There are several ways of implanting the stimulator. The initial implantation of the trial is generally done when you are awake so that you can determine if the stimulator is covering the appropriate spot of the spinal cord and is giving you pain relief.
Pioneer physicians place a trial lead using a spinal needle during a procedure performed at an outpatient ambulatory surgical center.
postoperative care following the insertion of a spinal cord stimulator trial lead
You are generally discharged on the same day or the following day of the procedure. You should keep the dressing very clean and dry. Do not take any blood thinner of any sort until the trial leads are removed, including Coumadin, Eliquis, or aspirin in any form.
risks and complications of a spinal cord stimulator
The risks of inserting a spinal cord stimulator are low. The potential risks include spinal headache, bleeding, infection, injury to nerves, injury to the spinal cord, paralysis, and death. The risk increases dramatically if the patients have any blood thinners in their system before or during the trial period.
SPINAL CORD STIMULATION
Spinal cord stimulation is a technology that can be used as a last resort to control chronic pain unresponsive to other measures. In this procedure, a very thin wire is passed to the outside of the spinal lining. Very low levels of electrical current are sent through this wire by a miniature generator controlled by the patient. The temporary procedure, or “trial,” is done in an operating room with anesthesia with a minimally invasive technique that does not require any incision. If successful in controlling an individual’s pain, a more permanent stimulator is surgically placed at a later date.
The science behind spinal cord stimulation has progressed rapidly over the past 30 years, and this procedure is now widely accepted as a treatment for many different types of pain syndromes. Some conditions that can be treated with this technology include failed back surgery, arthritic spinal pain, pinched nerves, spinal stenosis, CRPS (Complex Regional Pain Syndrome), peripheral vascular disease, and pain from chronic nerve damage.
DRG (Dorsal Root Ganglion) Stimulation is a related technology which is also performed by Pioneer physicians. In consultation, we can help determine whether either of these modalities are appropriate for your condition and which would be more effective.
PRE AND POST INSTRUCTIONS
Pre-Procedure Information
- Stimulator trials are performed in an ambulatory surgery center under conscious sedation (anesthesia). Expect to avoid eating and drinking for several hours before the procedure – the ambulatory surgical center will inform you of specific guidelines.
- The following medications are “blood thinners” of one sort or another and must be avoided before the procedure:
Aspirin
Aspirin and all aspirin containing medications (Anacin, Ascriptin, Bayer, Bufferin, Ecotrin, Excedrin, Pentasa, and others) – Stop 7 days prior to your procedure.
All medications listed below should be stopped 3 days prior to your procedure:
NSAIDs (NON-STEROIDAL ANTI-INFLAMMATORIES)
- Choline and magnesium salicylates (CMT, Tricosal, Trilisate)
- Choline salicylate (Arthropan)
- Diclofenac potassium (Cataflam)
- Diclofenac sodium (Voltaren, Voltaren XR)
- Diclofenac sodium with misoprostol (Arthrotec)
- Diflunisal (Dolobid)
- Etodolac (Lodine, Lodine XL)
- Fenoprofen calcium (Nalfon)
- Flurbiprofen (Ansaid)
- Ibuprofen (Advil, Motrin, Motrin IB, Nuprin)
- Indomethacin (Indocin, Indocin SR)
- Ketoprofen (Actron, Orudis, Orudis KT, Oruvail)
- Magnesium salicylate (Arthritab, Bayer Select, Doan’s Pills, Magan, Mobidin,
- Mobogesic)
- Meclofenamate sodium (Meclomen)
- Mefenamic acid (Ponstel)
- Nabumetone (Relafen)
- Naproxen (Naprosyn, Naprelan)
- Naproxen sodium (Aleve, Anaprox)
- Oxaprozin (Daypro)
- Piroxicam (Feldene)
- Salsalate (Amigesic, Anaflex 750, Disalcid, Marthritic, Mono-Gesic, Salflex,
- Salsitab)
- Sodium salicylate (various generics)
- Sulindac (Clinoril)
- Tolmetin sodium (Tolectin)
This is a partial list. If you are unsure whether you are taking an NSAID, please call us.
Please notify our office if you are on any of the medications listed below. These will probably need to be held for several days prior to your injection.
- Warfarin (Coumadin)
- Acenocoumarol
- Heparin
- Low molecular weight heparin: Enoxaparin (Lovenox)
- Dalteparin
- Fondaparinux
- Clopidogrel
- Prasugrel
- Ticagrelor
- Cangrelor
- Dabigatran
- Rivaroxaban (Xarelto)
- Apixaban (Eliquis)
- Edoxaban
- Abciximab
- Eptifibatide
- Tirofiban
- You will need to be driven home from the procedure. A friend or family member should be present to hear instruction on the operation of the stimulator after the procedure
Post-Procedure Instructions
- Do not take any of the medications listed above until the stimulator wires are removed.
- You will probably be sore for 1-2 days after the procedure. Talk to your physician about which medications you can take for increased pain.
